Preventing blood clots after hip or
knee replacement surgery
This booklet contains information for those who have been prescribed ELIQUIS® (apixaban) after a hip or knee replacement surgery
Carefully read the information in the patient information leaflet
YOU CAN FIND MORE INFORMATION AT:
www.1177.se
www.eliquispatient.se
You have received this booklet because your doctor has prescribed Eliquis® or you in order to prevent blood clots after a hip or knee replacement surgery.
Eliquis® will play an important role in your recovery by preventing the formation of blood clots. This booklet explains how it works and gives you some tools as a help during this period. You should also read the package information leaflet in the medicine pack. You can also find it on www.fass.se . You can get more information about the treatment with Eliquis®, practical advice and information material at www.eliquispatient.se
1. Blood clot (thrombus) 2. Vein
WHAT IS VENOUS THROMBOEMBOLISM?
The word “venous” indicates that something is related to the veins (the blood vessels that transport the blood back to the heart). A thrombus occurs when a blood vessel, which transports blood around in the body, is blocked by a blood clot. If a blood clot comes loose from the place where it was formed and follows the blood until it gets stuck in a narrower blood vessel elsewhere in the body, it is called an embolism.
A deep vein thrombosis (DVT) is a blood clot formed in the deep veins of the legs that pass through the muscles of the calves and thighs.
A deep vein thrombosis can block the blood flow of the vein wholly or partially, and cause symptoms such as pain, tenderness and swelling of the calf. Sometimes the calf becomes warm and red, in other cases no symptoms are noticed at all and the DVT is not diagnosed until a complication occurs, like a pulmonary embolism (blood clot in the lung).
Common symptoms of a blood clot in a leg:
the calf swells and becomes warm, sometimes also red or discoloured
the leg can feel heavy
the leg is aching, especially when walking and using the calf muscle
the calf is tender and tense if it is squeezed
superficial blood vessels on the leg may be more visible and feel tender
mild fever
It is important that you receive treatment for your blood clot since it may otherwise dislodge and be transported to the lungs, which may lead to difficulty in breathing.
In a pulmonary embolism, part of a blood clot breaks loose from a deep vein thrombosis and is transported to the narrower vessels in the lungs and gets stuck there. This causes it to block blood flow to a part of the lung. The symptoms of a pulmonary embolism are chest pain, respiratory distress, cough or a stitch in the side of the chest when breathing. If you experience such symptoms, you must contact a healthcare provider immediately.
Venous thromboembolism (VTE) is a term that includes both deep vein thrombosis and pulmonary embolism.
Blood clots that are formed in the veins of the legs or the pelvis may dislodge and be transported with the blood and then get stuck in the lungs. Sudden respiratory distress, cough or a stitch in the side of your chest when breathing may indicate that a blood clot has followed the blood to the lungs and has gotten stuck.
WHAT IS THE CAUSE OF VENOUS THROMBOEMBOLISM?
Blood coagulation is a natural process that stops bleeding. Movement of the leg muscles helps to push back the blood through the deep leg veins to the heart, so that a normal blood flow is maintained. If the blood starts to flow slower through the veins, it may coagulate and form blood clots. This happens more often during periods of reduced mobility, such as during and after surgery. The risk of such blood clots also increases after major surgery, since the blood’s ability to clot increases when the body tries to stop the blood loss and heal the blood vessels that were damaged during the surgery.
Even if not everyone who has surgery gets a blood clot, the condition can become serious for the person who is affected. This is why it is really important to try to prevent these blood clots from forming at all.
HOW CAN VENOUS THROMBOEMBOLISM BE PREVENTED?
Sitting still, smoking and being overweight are some of the factors that can increase the risk of getting a blood clot. The risk of blood clots can be reduced in the following ways:
Leg and foot movements: A physiotherapist will give you an exercise program that you should follow after the surgery. By exercising the foot and leg muscles, you help maintain a normal blood flow in the deep veins. Stretch and bend your feet as often as you can. It is best to stand up and do toe push-ups, if you are able to.
Weight: If you are overweight, it is positive if you can reduce your weight.
Tobacco: Avoid smoking.
Blood clot inhibitors (anticoagulants): These medicines reduce the blood’s ability to clot so that the risk of blood clots is reduced. Some agents are given as injections, while others are taken as tablets or capsules.
Your doctor may have chosen one or more of these preventive measures to reduce the risk of venous thromboembolism. Discuss with your care team if there is something else that you need to think about in order to reduce the risk of blood clots.
ABOUT ELIQUIS®
Why has your doctor prescribed Eliquis® for you?
Eliquis® is used in adult patients to prevent the forming of blood clots after a hip or knee replacement surgery.
Eliquis® contains the active substance apixaban and belongs to a group of medicines called anticoagulants (blood clot inhibitors).
Eliquis® helps prevent blood clots from forming by blocking one of the substances that causes the blood to coagulate (factor Xa).
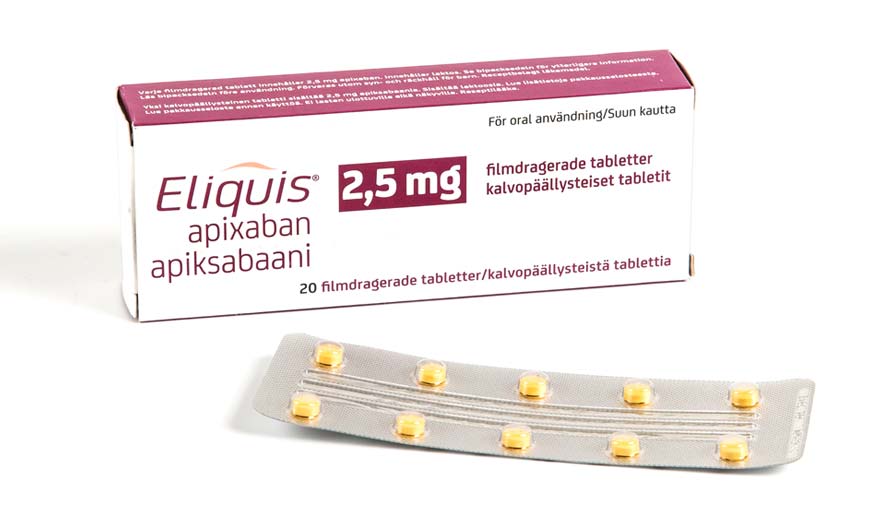
How should Eliquis® be taken?
You should always take Eliquis® exactly as instructed by your doctor. Consult your doctor or pharmacist if you are not sure.
For preventative treatment of thrombosis in connection with a hip and knee replacement surgery, the usual dose for Eliquis® is one 2.5 mg tablet twice a day, for example one in the morning and one in the evening. Try to take the tablets at the same time every day.
You should swallow the Eliquis® tablet with a glass of water or you can crush it and mix it with water. You can take it with or without food. It is ok to keep the Eliquis® tablet in a pill organiser box.
How long will the Eliquis® treatment last?
The length of treatment depends on the type of surgery you have undergone. Always follow the doctor’s instructions. Do not stop taking your medication unless your doctor tells you to do so. Always tell your doctor, dentist or nurse that you are taking Eliquis®.
FAQ
What should I do if I forget a dose?
If you forget to take a dose of Eliquis®, take the tablet as soon as you remember. Then take the next Eliquis® tablet at the usual time, and continue as normal. If you are unsure, ask your doctor or pharmacist.
What should I do if I have taken too much Eliquis®?
Talk to your doctor immediately if you have taken more than the prescribed dose of Eliquis®. Bring the medicine pack to the doctor, even if there are no tablets left. If you take more Eliquis® than recommended, you are at increased risk of bleeding.
Things to keep in mind when taking Eliquis®
Be sure to tell your doctor if you are taking any other medicines, including over-the-counter medicines and herbal medicines (e.g. St. John’s Wort). Some medicines and supplements may interfere with the blood clot inhibiting effect of Eliquis® and either increase the risk of bleeding or cause the drug to be less effective. You will find a complete list of medicines that may affect Eliquis® in the package information leaflet in the medicine pack.
You should not take Eliquis® if you are pregnant, breastfeeding or have a liver disease or bleeding disorder. Therefore, please tell your doctor if any of these apply to you.
POSSIBLE SIDE EFFECTS
Like all medicines, Eliquis® can cause side effects.
You can read more about side effects in the package information leaflet that comes with the drug packaging.
Eliquis®, as well as other blood clot inhibiting drugs, increases the risk of bleeding, including serious ones that require immediate medical attention.
Other occurring side effects are bruising, blood in the urine (which stains it pink or red) or nosebleeds. Nausea may also occur. If there is unexpected bleeding, you should contact your doctor or nurse.
Good luck with your rehabilitation!
NOTES
Eliquis® belongs to a group of medicines called anticoagulants (blood thinners). This medication helps prevent blood clots from forming by blocking factor Xa, which is an important component in the clotting of blood. The active substance in Eliquis® is called apixaban. Eliquis® is available as film-coated tablets in strengths of 2.5 mg and 5 mg. Eliquis® is used for adults: 1. To prevent blood clots (deep vein thrombosis, DVT) from forming after a hip or knee joint surgery. 2. To prevent blood clots from forming in the heart of patients with an irregular heart rhythm (atrial fibrillation) and at least one more risk factor. Blood clots can come loose and be transported to the brain and cause a stroke, or to other organs and prevent normal blood flow to these organs. 3. To treat blood clots in the leg veins (deep vein thrombosis) and in the blood vessels of the lungs (pulmonary embolism) and to prevent blood clots from recurring in the blood vessels in the legs and/or the lungs. Do not use Eliquis® if: you are allergic to apixaban or any of the other ingredients in this medicine, you have an ongoing bleed, you have a disease in a body organ that increases the risk of severe bleeding (such as current or recent ulcers in the stomach or intestine, recent bleeding in the brain), you have a liver disease that leads to increased risk of bleeding (hepatic coagulopathy), you are taking medicines to prevent blood clots (e.g. warfarin, rivaroxaban, dabigatran or heparin), except when changing anticoagulation treatment, or while you have a venous or arterial catheter and you are receiving heparin to keep it open, or if a tube is inserted into the vein (catheter ablation) to treat irregular heart rhythm (arrhythmia). Talk to your doctor, pharmacist or nurse before you take this medicine: if you have a serious kidney disease, or if you are on dialysis, if you have a problem with your liver or have had previous problems with your liver, if you have an artificial heart valve or if you know that you have a disease called antiphospholipid syndrome (a disturbance in the immune system that increases the risk of having blood clots). For full information about Eliquis®, carefully read the package leaflet that accompanies the pack (see also www.fass.se).
Bristol Myers Squibb, 08-704 71 00. Pfizer AB, 08-550 52 000.
Version 4
432SE2100916-01, 432SE2008250 PP-ELI-SWE-1621 OCT 2020